Is Sugar Making Your Chronic Pain Worse? (What Most Doctors Don’t Tell You)
- Dr. Jason Winkelmann

- 1 day ago
- 9 min read

TL;DR
Sugar does not just “cause inflammation.” It changes how your body produces energy, how your nerves regulate pain, how your tissues heal, how your blood vessels function, and how your immune system behaves. For chronic pain sufferers, that matters because pain is not just about where it hurts. It is about the physiological environment surrounding the tissues, nerves, and brain. Sugar is rarely the only cause of chronic pain, but it is often one of the most common reasons the body stays inflamed, under-repaired, and overly reactive.
What Patients Are Usually Told
Most chronic pain sufferers are told something vague and unhelpful about sugar.
Usually, it is one of two things:
Either they are told sugar is bad because it causes inflammation, or
They are told diet does not really matter that much unless they are diabetic or trying to lose weight.
Both explanations sound reasonable for a moment.
It is true that sugar can contribute to inflammation. It is also true that excess sugar is associated with obesity, diabetes, and cardiovascular disease. But this is where the explanation becomes incomplete for chronic pain sufferers.
Because the real issue is not whether sugar is generically unhealthy. The real issue is whether sugar creates a body that is less capable of healing and more likely to produce pain.
That is a much more important question, and it is the one most patients are never taught to ask.

Pain Is Not The Problem
Pain is a symptom. It is not the underlying problem itself.
That distinction matters because chronic pain does not persist simply because tissues are damaged. It persists because the systems responsible for repairing tissue, calming inflammation, regulating nerves, maintaining blood flow, and producing cellular energy are no longer functioning the way they should.
When those systems are disrupted, your body uses pain as a way to get your attention. It is the ultimate symptom, one that is impossible to ignore.
This is why chronic pain can flare without a new injury. It is why symptoms can worsen even when imaging looks the same. And it is why so many sufferers feel like their body has become unpredictable.
The tissues matter, of course. But the tissues are living inside a metabolic, inflammatory, vascular, and neurological environment.
Sugar influences all of those environments.
So the better question is not, “Does sugar cause pain?”
The better question is, “What is sugar doing to the systems that regulate pain?”
The Physiology Most Patients Are Never Taught
Most people think of sugar as fuel.
That is technically true, but it is a very shallow explanation.
What many patients are never told is that how your body creates energy matters just as much as how much energy it has available. And when sugar intake is high, the body is pushed toward a metabolic state that is less stable, less efficient, and much more inflammatory.
Sugar Changes How Your Mitochondria Produce Energy
Your mitochondria are the energy-producing structures inside most of your cells. Their job is to produce ATP, which is the usable energy your body needs for everything from tissue repair and nerve stability to immune regulation and detoxification.
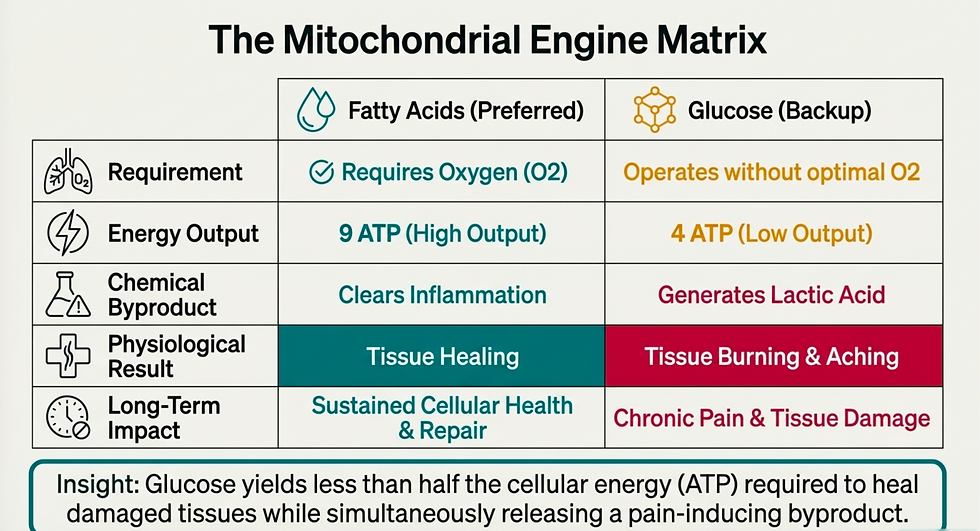
Your mitochondria can produce energy in one of two ways:
Using its preferred fuel source of fatty acids (dietary fat) and oxygen. This method produces 9 ATP per molecule of fatty acids.
Using its backup fuel source of glucose without oxygen. This option produces 4 ATP per molecule of glucose.
However, the second option also produces lactic acid. This is produced most notably during exercise. It is responsible for the burning and aching sensation you feel in your muscles. Under normal circumstances, lactic acid is a good thing. It is a signaling molecule that tells your body to repair the damage and make those tissues stronger. But with chronic pain, you get all the harm without any of the benefits.
What this means for patients is that a high sugar diet can leave the body producing less efficient energy while simultaneously creating more of the chemistry associated with pain and fatigue.
That is a terrible combination for someone already struggling to recover.
Sugar Destabilizes Blood Sugar, And Unstable Blood Sugar Is A Stress Signal
Most patients are taught to think about blood sugar in the context of diabetes.
That is another incomplete explanation.
Blood sugar instability affects much more than diabetic risk. It affects cortisol, inflammatory signaling, oxidative stress, vascular tone, and nervous system reactivity.
In other words, it changes how calm or how reactive your body becomes.
When blood sugar spikes, inflammatory signaling tends to increase.
When blood sugar crashes, stress hormones rise and oxidative stress increases.
Either way, the body is pulled away from a stable healing environment.
This is one reason so many chronic pain sufferers notice they feel worse after certain meals, worse when they skip meals, or worse when their diet is built around processed carbohydrates. They often assume they are imagining it because no one has ever explained the physiology.
They are not imagining it.
Their nervous system is responding to a less stable internal environment.
And a less stable internal environment almost always means more pain.

Sugar contributes to insulin resistance, and insulin resistance affects pain signaling
Insulin is not just a blood sugar hormone.
It is also a signaling molecule with major effects on metabolism, inflammation, and nerve health. Under healthy conditions, insulin helps move glucose into cells where it can actually be used rather than left circulating in the bloodstream, where it becomes more damaging.
But when sugar and carbohydrate intake are consistently high, cells can become less responsive to insulin, leaving glucose floating around your bloodstream. This is insulin resistance.
At that point, the problem is no longer just sugar.
The problem becomes signaling.
Tissues become harder to nourish properly. Inflammation becomes easier to sustain. Nerves become more vulnerable. The body becomes less flexible metabolically and more prone to exaggerated responses.
This is especially relevant in chronic pain because insulin also has neurotrophic effects, meaning it helps support healthy nerve function. When that signaling is impaired, peripheral nerves can become more irritable and the central nervous system can become easier to sensitize.
What this means for patients is that insulin resistance can quietly amplify pain long before anyone tells them they have a blood sugar problem.

Sugar Creates Advanced Glycation End Products, And Those Damage Tissue Quality
This is one of the most important mechanisms almost no one explains well.
Sugar does not just circulate in the bloodstream and then disappear. It can bind to proteins and change their structure. These altered compounds are called advanced glycation end products, or AGEs.
That matters because proteins only work correctly when their shape is intact. Their structure determines how they bind to receptors, how they signal, how they form connective tissue, how they repair damaged areas, and how they help the body maintain resilience. When sugar alters that structure, those proteins stop doing their jobs well.
Now imagine trying to repair muscles, ligaments, tendons, cartilage, fascia, and nerves using damaged building materials.
That is part of what chronic pain patients are up against.
AGEs also tend to accumulate in the exact tissues chronic pain sufferers already depend on most for stability and function: connective tissue, neuromuscular tissue, cartilage, and nerves.
What this means for patients is that sugar does not just cause pain in the short term. Over time, it can make tissues less resilient, less repairable, and more mechanically and neurologically sensitive.
This is one reason hyperalgesia becomes such a problem in chronic pain. Things that should only hurt a little start hurting a lot. Things that should not hurt at all can begin to feel painful.

Sugar Worsens Gut-Driven Inflammation
Most patients think the gut only matters if they have obvious digestive symptoms.
But the gut is not just a digestive organ. It is one of the central regulators of immune activity, inflammation, barrier integrity, nutrient absorption, and neurotransmitter production in the body.
Sugar feeds the wrong microbial balance.
When that happens, beneficial bacteria tend to decline and more inflammatory organisms are favored. This creates a state of dysbiosis, which means the gut becomes less protective and more inflammatory.
That matters for chronic pain because the gut helps regulate immune tone, inflammatory load, nutrient absorption, and even the production of neurotransmitters involved in mood, stress regulation, and pain processing.
What this means for patients is that sugar can make chronic pain worse without causing obvious digestive symptoms first. You do not have to feel bloated every day for your gut to be contributing to a more inflammatory, pain-amplifying physiology.
Sugar Impairs Blood Flow, And Poor Blood Flow Slows Healing
Your tissues need oxygen, water, nutrients, hormones, and immune cells. They also need efficient removal of inflammatory waste and metabolic debris. Blood flow is how that happens.
When sugar intake is chronically high, blood vessels do not function as well. Endothelial health worsens. Nitric oxide signaling becomes less balanced. Blood pressure regulation becomes less efficient. Plaque formation becomes more likely. Microcirculation becomes less effective.
Now you have a delivery problem.
And if tissues are not receiving what they need, they cannot heal well, no matter how many symptom-focused treatments you throw at them.
Less oxygen reaches muscles. Less nutrition reaches connective tissue. Less waste is removed from inflamed regions. Recovery slows down.
What this means for patients is that sugar can help create the exact low-healing environment that keeps pain going.

Sugar Worsens The Fatigue-Pain-Stress Cycle
Anyone with chronic pain knows that fatigue is rarely just “being tired.” It feels more like your system is underpowered.
Your threshold for stress drops. Your pain becomes harder to tolerate. Your sleep becomes less restorative. Your brain feels foggier. Your body feels heavier.
Sugar contributes to that state by destabilizing energy production and disrupting cortisol rhythms. Many patients end up feeling tired during the day, wired at night, hungry at strange times, and more inflamed overall.
This is one reason patients often feel like stress, sleep, fatigue, and pain are all tied together in one knot.
Because physiologically, they are.
Why Carbohydrates Can Be Just as Problematic as Sugar
Up until this point, we have just been talking about sugar. In reality, carbohydrates also fit into this category. That is because all carbohydrates can get converted into glucose in your body.
Carbohydrates come in three forms:
Monosaccharides
Oligosaccharides
Polysaccharides
The first two are considered simple carbohydrates, which you have likely been told are the bad carbs. Polysaccharides are complex carbs, which you have probably been told are good carbs.
Unfortunately, this is an oversimplification that is hurting you.
All simple carbs, whether fructose (from fruit), maltose (from grains), lactose (from dairy), or sucrose (table sugar), can be converted into glucose in the body through a process known as gluconeogenesis.
Complex carbs are considered good because they get converted into glycogen, your sugar storage molecule found in your muscle and liver cells. When glucose is stored as glycogen it can't harm your body. However, if you are more sedentary and not using that glycogen, especially because of your pain, glycogen can also be converted to glucose through glycogenolysis.
Therefore, any carbohydrate can be just as detrimental as sugar for the chronic pain sufferer.

Why Standard Treatments Often Fail
Most standard chronic pain treatments aim at the symptom.
They numb tissue. Suppress pain signals. Reduce inflammatory chemistry temporarily. Relax muscle tone for a few hours. Calm a flare enough to get through the day.
Sometimes that is useful. Sometimes it is necessary.
But those treatments do not meaningfully change the metabolic environment if the body is still being pushed toward unstable blood sugar, poor mitochondrial function, glycation damage, gut dysbiosis, vascular dysfunction, and increased nerve sensitivity.
This is why so many chronic pain sufferers feel like treatments help, but never really move the needle.
The problem is not always that the treatment failed completely.
The problem is that the physiology underneath the pain was still working against recovery.
Why Your Tests Can Look Normal While Sugar Still Makes You Worse
This is one of the most frustrating parts for patients.
You may not have diabetes. Your imaging may be unchanged. Your standard inflammatory markers may not look dramatic. Nothing obvious jumps off the page.
And yet you know your pain is worse when your diet is worse.
That does not make you dramatic. It means physiology is often subtler than the way conventional testing is interpreted.
Mitochondrial dysfunction does not show up well on routine labs and imaging. Early insulin resistance is often missed. Dysbiosis can exist without severe GI symptoms. Glycation damage accumulates quietly. Nervous system sensitization is functional long before it becomes obvious structurally.
So yes, your tests can look “fine” while sugar is still making your system more inflamed, more reactive, and harder to heal.
Reframing the Question
The wrong question is: Is sugar bad for chronic pain?
That question is too small.
The better question is: Is sugar creating a physiological environment where my body cannot heal efficiently and my nervous system becomes easier to irritate?
That is the real issue.
For many chronic pain sufferers, sugar is not the original cause of the problem. But it is often one of the strongest reasons the problem stays amplified.

Written By:
Dr. Jason Winkelmann
Naturopathic doctor, Chiropractor, Chronic Pain Specialist, and Educator
Frequently Asked Questions
Is sugar really worse for chronic pain patients than for the average person?
Often, yes. Not because chronic pain sufferers are weaker, but because their systems are already more sensitized. When your nervous system, immune system, metabolic system, and vascular system are already under strain, the same dietary insult tends to hit harder.
Are carbohydrates just as bad as sugar?
Many of them can have very similar effects. Simple carbohydrates raise blood sugar rapidly, and even more complex carbohydrates can become problematic if overall intake is high and energy demand is low enough that stored glycogen is simply converted back into glucose rather than used.
Is fruit a problem too?
Fruit comes with fiber, vitamins, minerals, and beneficial plant compounds, which makes it different from soda or candy. But fructose is not metabolically irrelevant. For some chronic pain patients, even healthier carbohydrate sources may still need to be evaluated in the context of blood sugar stability and symptom patterns.
If I reduce sugar, will my chronic pain go away?
Not necessarily. Chronic pain is almost always multi-factorial. But lowering sugar can remove one major source of metabolic stress, inflammatory signaling, vascular dysfunction, tissue glycation, and nervous system irritation. For some patients, that produces meaningful improvement. For others, it is one foundational piece that allows all other treatments to work better.



Comments